[ad_1]

Doctor holding a red heart
© Blue Planet Studio / stock.adobe.com
It is known that the prognosis of cancer treatment depends on plenty of factors, and last but not least, cardiotoxicity (heart damage) caused by chemotherapy. According to cancer statistics, breast cancer consistently ranks first among the causes of death in women globally. Studies in patients with breast cancer receiving chemotherapy have shown an increase of up to 2.2 times in the relative risk of developing fatal cardiovascular complications.
Chemotherapy in breast cancer patients involves using several classes of pharmaceuticals, primarily anthracyclines, and targeted treatments – monoclonal antibodies, low molecular weight tyrosine kinase inhibitors, and proteasome inhibitors. In patients treated with anthracyclines, complications usually develop within the first year after stopping chemotherapy and proceed as progressive chronic heart failure, up to the development of dilated cardiomyopathy, where the heart walls become stretched and thin so that they cannot pump blood effectively.
Trastuzumab, the mainstay of treatment for HER2-positive breast cancer, reduced death rates from breast cancer by one-third but did not meet expectations concerning severe cardiac complications. Up to 3% of patients treated with trastuzumab experience severe cardiotoxic complications, while the combined use of anthracycline and trastuzumab leads to a sevenfold increase in chronic heart failure risk.
Illustration of breast cancer
© Axel Kock / stock.adobe.com
One of the best solutions to prevent the adverse heart effects of chemotherapy is the timely administration of cardiac protectors with proven effectiveness. Angiotensin-converting enzyme (ACE)-inhibitors, beta-blockers, and other specified medicines can normalize left ventricular ejection fraction (how much blood is pumped to the body) in 82% of patients, thus significantly improving the prognosis of the underlying disease.
The problem is so urgent that a new discipline – cardio-oncology – has been created by leading world experts who regularly publish their considered opinion on the prevention, diagnosis, and treatment of cardiovascular toxicity during anticancer treatment. We expect the first European guide on cardio-oncology to be published soon. Previously published expert papers include consolidated statements on the early diagnosis and prevention of cardiotoxicity in cancer patients.
Currently, the management of cardiotoxic effects of chemotherapy has not yet come into practice in Kazakhstan. In this regard, we have developed our multidisciplinary project titled “Development of a PRogram for Early DIagnosis and treatment of CArdiotoxic complications caused by chemoTherapy for brEast cancer“ (PrEDiCaTE).
Based on the latest observations and achievements in cardio-oncology, our research aims to develop a program for early diagnosis and treatment of the heart complications of breast cancer chemotherapy. In the first part of the study, we assessed all available data from our regional cancer registry for 2018-2019. We revealed that in every tenth patient treatment was interrupted due to chemotherapy adverse effects, and six out of ten faced heart complications.
In the prospective part of the study, we will estimate the predictive value of the blood levels of biomarkers (damage, inflammation, neurohormonal activation, oxidative stress, fibrosis, and thrombosis) in patients with breast cancer. The usefulness of these markers in detecting early heart dysfunction will be assessed using advanced heart imaging (heart global longitudinal strain [GLS] assessment).
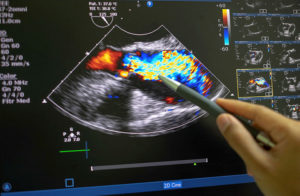
Echocardiography (ultrasound) machine
Women of any age who have a verified diagnosis of breast cancer at any clinical stage can participate if admitted to the West Kazakhstan Marat Ospanov Medical Unversity. They should be receiving chemotherapy with anthracyclines or targeted therapy and not have pre-existing symptoms of heart failure within the 30 days before admission.
On signing the informed consent, all selected participants were divided into four large groups depending on their risk of cardiovascular complications. They were provided with cardioprotective treatment if needed.
At the start of the study and then after 3, 6, 9, and 12 months, participants undergo heart imaging (echocardiography: Holter monitoring, speckle tracking – ultrasound for GLS assessment) and blood was collected to measure the levels of cardiac troponin (cTnI), brain natriuretic peptide (BNP), C-reactive protein (CRP), myeloperoxidase (MPO), Galectin-3 (gal-3) and D-dimer. The data collection lasts about 2 years in total (22 months).
What is the novelty of our research?
The key difference of our project is that we are studying all currently known markers indicating a decrease in the contractile function of the heart. Our goal is to select by comparative analysis those markers that are the first to indicate cardiac dysfunction, detected by echocardiographic methods, particularly speckle tracking. Speckle tracking is a relatively expensive method for studying heart function while measuring biomarkers is much more affordable. We hope to develop a practical algorithm for early diagnosis and prevention of chemotherapy cardiotoxicity, thus enabling patients to complete their course of treatment.
[ad_2]
Source link