[ad_1]
Maternal vaccination against respiratory infections is crucial to protect pregnant women as well as their newborns after birth. In Australia, influenza and pertussis vaccinations are free to all pregnant women, but uptake is sub-optimal with variations by region, socioeconomic status, and cultural background. In this blog post, the author of a new paper in BMC Pregnancy and Childbirth discusses inequities in vaccine uptake among three groups at higher risk of complications from vaccine-preventable infections.
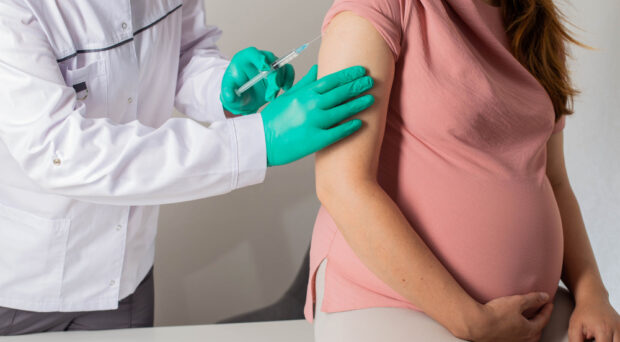
Maternal vaccination
Pregnancy and early infancy are increased risk periods for severe adverse effects of respiratory infections. Influenza vaccines (IIV) and whooping cough (pertussis) vaccines are recommended and free to every Australian pregnant woman to combat these infections during pregnancy, and the vaccines provide protection for young infants as well for approximately the first six months of life, through the transfer of maternal antibodies across the placenta.
Because there is no central, national system in Australia that routinely monitors maternal vaccination uptake, it is unclear whether there is equitable distribution of these vaccines among our diverse populations. This is important because despite being recommended and free in Australia for decades, the overall uptake of IIV in pregnancy varies greatly between the different states and territories. Uptake generally remains sub-optimal, and we need to be confident that those with higher risk factors for infection in pregnancy and early infancy are being offered and provided vaccination. These risk factors include people with co-morbidities, living in remote regions, lower socio-economic status, inadequate housing, decreased rates of exclusive breastfeeding, and limited access to culturally safe and appropriate, affordable health care.
Existing inequities
Our previous work found that rates of pertussis vaccination in pregnancy were higher than they were for IIV, and that pertussis vaccination in pregnancy was a key driver for having IIV in pregnancy. But we also found that pertussis vaccination was considerably lower (17%) among Aboriginal and/or Torres Strait Islander pregnancies (respectfully referred to as First Nations) compared to other Australians (54% vs 71%). This was concerning because First Nations women and infants in Australia bear a disproportionately higher burden of respiratory diseases compared to non-Indigenous women and infants, which is a consistent finding in other countries’ Indigenous populations.
Vaccination against these infections has to be prioritized in these groups as a key public health strategy in preventing severe disease in pregnancy and early infancy and is the benchmark of equitable healthcare.
In our new paper in BMC Pregnancy and Childbirth, we sought to understand these findings further, so we explored the equity of maternal IIV and pertussis vaccination for three Australian groups between 2012-2017: First Nations women; women from culturally and linguistically diverse (CALD) backgrounds; and women living in remote areas or areas considered socio-economically disadvantaged. Our cohort of 445,590 individual pregnancies from the Northern Territory, Queensland and Western Australia comprised of 29,181 First Nations women (6.5%), 93,561 women from CALD backgrounds (20.9%), and 322,848 other Australian women (72.4%).
Over the six years we found that although maternal vaccination rates were steadily increasing over time, overarching inequity persisted in participants who a) identified as First Nations, b) lived in remote areas, and c) lived in areas considered the highest in disadvantage. Compared with the other groups, First Nations women were less likely to have received both of the recommended maternal vaccines whereas women from CALD backgrounds were more likely to have. Women living in the highest areas of advantage were more likely to have received both vaccines during pregnancy too.
We know the increased risk factors for acquiring influenza or pertussis infections are living in remote regions, lower socio-economic status, inadequate housing, and limited access to culturally safe and appropriate, affordable health care. Vaccination against these infections has to be prioritized in these groups as a key public health strategy in preventing severe disease in pregnancy and early infancy and is the benchmark of equitable healthcare.
What’s next?
We plan to reassess these outcomes using contemporary data to determine whether our study findings still hold true five years later. Acquiring these multiply linked, whole of population data is a slow process though, and as experts in our field, we believe that a national, maternal vaccination surveillance system is warranted. One that can provide ongoing, reliable, accurate and timely data on vaccination uptake, and identify areas in vaccine inequity, so that appropriate resources can be mobilized to address the areas of inequity.
 This paper is part of the ‘Disparities in access to sexual and reproductive health services’ Collection in BMC Pregnancy and Childbirth and BMC Women’s Health. You can see all of the papers in the Collection here.
This paper is part of the ‘Disparities in access to sexual and reproductive health services’ Collection in BMC Pregnancy and Childbirth and BMC Women’s Health. You can see all of the papers in the Collection here.
[ad_2]
Source link