[ad_1]

a)A sandstorm blows across the Nile in Sudan. Credit: Madin Adam 663 on Wikimedia Commons”
Without qualification, this article title may sound like a sci-fi horror scenario; “Urban malaria may be spreading via the wind”. Authored by Tovi Lehmann and colleagues, it implies that the parasites are bursting forth from their hosts’ circulation, with vapourised Plasmodium flying through the air in droplets, and penetrating the vulnerable via their respiratory system. However, this recent opinion piece is actually referring to the spread of the mosquito vector of Plasmodium malaria, although this clarification should not be too reassuring.
Many mosquito species can transmit the malaria parasite, and in different parts of the world some are more prominent transmitters than others.

Anopheles gambiae and Anopheles stephensi: two mosquitoes which may look similar but spread malaria in distinctive ways. Credit: Muhammad Mahdi Karim and CDC respectively on Wikimedia Common.
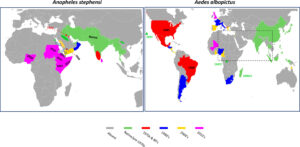
For example, in most of Africa the species Anopheles gambiae is the major malaria-giver, while in the Indian sub-continent it is Anopheles stephensi. This is not merely a technical note, as the different mosquitoes have distinct behaviours which impact how the parasite spreads. An. gambiae is a countryphile, making African malaria mostly a rural issue. In contrast, An. stephensi prefers urban environments, laying eggs in stagnant water containers around cities.
When a given mosquito vector moves into a new area, it can expose previously protected populations to the pathogen.
After a mysterious and unexpected malaria outbreak occurred in an East African city a decade ago, it led to the first identification of the Asian-native An. stephensi in the Horn of Africa. In the intervening years it has spread further around the continent, including Westwards. Africa already bears the greatest global burden of P. falciparum malaria, so it is of grave concern that An. stephensi is now spreading across this continent, potentially complementing An. gambiae as a vector. It is predicted that urban outbreaks, previously an irregular occurrence, could become much more likely. Given the spread, major cities such as Khartoum, Lagos, Abuja, Mogadishu, Nairobi, Mombasa, and Addis Ababa are all in the firing line.
So how did An. stephensi escape Asia? Lehmann and colleagues contend that the answer is deceivingly simple; they are carried by the wind.
This is more-or-less a refute to a previous hypothesis; that the vector was spread by maritime transport. There was good reason to believe the original suggestion; the first location An. stephensi was found in Africa was in the port town of Djibouti City. Secondly, An. gambiae reached Brazil in the 1930s, carried across the Atlantic by planes or boats. Additionally, the mosquitoes Aedes aegypti and Aedes albopictus (carriers of many viral diseases, such as dengue and Zika) spread globally over the 19th and 20th centuries due to international trade. In their native countries, the mosquitoes layed eggs in pools of stagnant water in, say, tyres. During the voyage, the eggs hatched and invaded where the ship had made landfall.
Lehmann and co. pointed out reasons why this is unlikely to be the best explanation for the recent spread of An. stephensi. While the Aedes eggs are highly resistant to drying out (desiccation) and can hatch when re-wetted, An. stephensi cannot resist desiccation, and hence are less suited for long trips at sea. The pattern of migration is also distinctive. Aedes albopictus travelled from Central and Western Asia around the world, including to isolated islands and regions far from their origin, such as the Americas. In contrast, An. stephensi has moved almost linearly outwards from its source: From Northern Arabia it transferred to Oman in the 90s, snaked around the peninsula into Yemen and Southern Arabia in the 00s, and then finally was observed in Djibouti City (2012) – which is indeed a centre of maritime travel but also geographical close to Arabia. Once in Africa, it continued on to the nearby countries of Sudan (2016), Ethiopia (2016), and Somalia (2019). In the last few years, the species has continued its invasion across the continent, including neighbouring Kenya (2022) and a ‘jump’ across the interior to Nigeria (2020).
With An. stephensi ill-equipped for maritime travel, and a pattern of travel that didn’t implicate long-distance trade routes, a better explanation was needed. That answer may have come from a paper by Huestis and colleagues in 2019 (as discussed in this previous BugBitten blog). By attaching gluey nets to balloons they created insect sampling stations which could operate a few hundred metres in the air. When they used these aerial sticky traps over several months in central Mali, they found mosquitoes, including the main African malaria vector An. gambiae, surprisingly high in the air. For blood feeding the insect must remain near the ground, but now we knew they could reach at least 300m into the sky.

By using the wind speed at these heights, and established measurements of maximum flight times, the experimenters could back-calculate a trajectory of the vertex-borne bugs, concluding that they could be travelling as far as 300km. Huestis and co.s’ experiment didn’t find any An. stephensi (so far the species hasn’t been found in Mali) but there is no reason to believe this species would be unable to travel this way. Indeed, this wouldn’t be the first flying insect known to transmit between the continents like this. The authors pointed out that locusts regularly migrate across the Red Sea with the wind’s assistance, inflicting massive damage to agricultural crops.
The trigger for the spread of this mosquito still needed explanation, and the authors suggest that urbanisation of the Arabian peninsula provides the answer. An. stephensi prefers cities, and this inclination may have been what protected Africa from its spread for so long. The Arab nations once provided a sparsely-populated buffer zone, then oil was discovered and the major Gulf metropolises emerged – creating city-size stepping stones to Africa. Perhaps the wind and urbanised refuges are also what’s driving An. stephensi to conquer new territory in South-East Asia, Sri Lanka, and Northern Iran, all of which have reported this species in regions in which it was previously presumed to be absent.
There hasn’t been continuous mosquito sampling in all the new areas and the intervening land, so it is possible that An. stephensi was there before and hadn’t been officially recorded. However, for the same reason, the flip side of this is almost a certainty; that An. stephensi has already reached countries where it has not yet been recorded. While Mnzava and colleagues in Tanzania stress the uncertainties over how much of an impact An. stephensi has made, and will make, they are certain that the surprise by which this expansion took the community is symbolic of the lack of adequate sampling.
With the ‘Asian’ malaria vector breaking into the new continent like a proboscis probing hungrily inside the skin, what does this theory mean for the future of public health in Africa? Lehmann and co. state that “it is hard to overstate the public health importance of this paradigm shift” for the introduction of An. stephensi. If they are right, blocking transmission is a lost cause; The wind cannot be controlled. However, what we do to tackle the new arrivals in recipient cities is within our power. Without the right methods, surveillance, and initiative, Africa may be burdened with a game-changing new antagonist in its battle against disease.
[ad_2]
Source link