[ad_1]
There is no doubt that COVID-19 has placed great stress on our healthcare system. In many areas of the world, healthcare systems neared collapse with the curtailment of elective and semi-elective services. The United States fared worse than many other developed nations. It has a population which is very resistant to public health strategies and vaccinations. Today it is 68th in the world in the number of individuals who have obtained a COVID-19 vaccine. The United States also has a private healthcare system which has been run for maximal financial efficiency. This system has a just-in-time supply chain and a nursing shortage which has existed for decades.
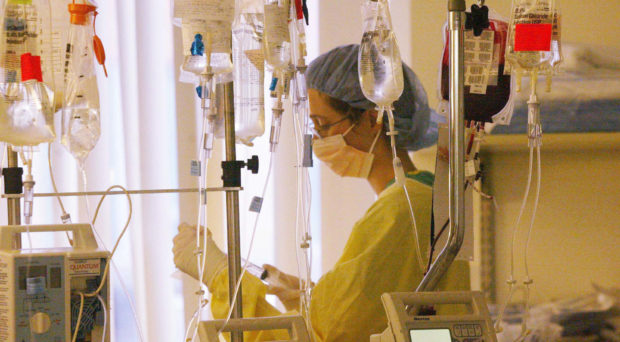
credit: Lisa R. Kyle
lisakylephotography.com
There is widespread agreement that system transformation must take place, but there appears to be little action. The free market and consumer choice are often touted as forces to drive healthcare quality, but for these to work, transparency and accountability are of prime importance.
In the United States, quality metrics for hospitals are publicly reported on Hospital Compare. These metrics generate data which both educates the consumer and are used in Federal financial incentive programs. Depending upon the program, hospitals can be either penalized or rewarded for their performance.
During the COVID-19 pandemic, the U.S. healthcare system neared collapse, in large part due to lean staffing and meager stockpiles of supplies. However, instead of transformation, it appears policymakers have assumed that facilities can do little to prevent safety lapses in the presence of COVID-19, and the Centers for Medicare and Medicaid (CMS) have decided to “risk” adjust quality metrics used in financial incentives. In the Hospital-Acquired Condition (HAC) Reduction Program, the Hospital Value-Based Purchasing (VBP) Program and the Hospital Readmission Reduction Program (HRRP), COVID-19 patient data have been suppressed in almost all metrics for fiscal year 2023. Also, the system which reports consumer assessment of our healthcare system is being paused for the VBP Program.
In the United States, this would include a large segment, possibly half of the population. No one knows for sure, since no one is actually counting
For the Readmission Reduction program, the exclusion applies to any patient admitted with pneumonia that has a COVID-19 diagnosis that is present on admission. Beginning in 2024, all six procedures monitored for readmission penalties will be risk-adjusted for COVID-19 if the patient has a history of COVID-19 within the last 12 months. In the United States, this would include a large segment, possibly half of the population. No one knows for sure, since no one is actually counting (see interview with Frazier Beatty).
In addition, the five CDC National Healthcare Safety Network (NHSN) healthcare-associated infection measures for the HAC Reduction Program are suppressed for fiscal year 2023, 2024.
Facility performance on these incentive programs are publicly reported by major news outlets.
For the public, the risks of Long COVID and the frequent and severe sequelae of COVID-19 are downplayed, but for healthcare facilities, patients who have had COVID-19 in the last 12 months are viewed as high-risk and adverse outcomes are not uniformly included in financial incentive programs.
Learning to live with COVID-19 means investing and strategizing to reduce risk and mitigate adverse outcomes
Learning to live with COVID-19 does not mean learning to accept a higher rate of adverse outcomes, death, and disability. Learning to live with COVID-19 means investing and strategizing to reduce risk and mitigate adverse outcomes.
We, thus, sought to ask the question: Is the high rate of adverse events encountered by patients during the COVID-19 pandemic an unavoidable outcome of COVID-19 or an avoidable system failure? If the latter, then risk-adjustment of financial incentives would be ill advised, since it would normalize deviance and effectively penalize hospitals who invest in the prevention of adverse events in COVID-19 patients.

VA Hospital
Public domain image
To help answer this question, in our recent paper, we compared rates of MRSA hospital-onset infections in the Veterans Health Administration (VHA) with those in the private sector as recorded in the CDC’s NHSN reporting system. To our surprise, there was a 100 percentage point difference. The rates in the private system were 16.8% above their baseline, as the VHA system maintained an 83.6% reduction.
Some will argue that this is comparing apples and oranges, but the VHA system treated COVID-19 patients and during the peak of the pandemic even hospitalized non-veterans from the private sector. And VHA patients are a higher risk older population than the average patient served by the private sector.
In addition, patients will only develop an MRSA infection if they are exposed to the organism. During peaks of COVID-19, many hospitals in our private system had extreme staff shortages and were too often staffing whole wards with agency or temporary nurses who were unfamiliar with hospital protocol and the hospital’s electronic medical record systems. In contradistinction, the VHA was able to deploy staff to assist non-VHA and private facilities.
Active surveillance is key to the prevention of infectious disease, whether it is COVID-19, CRE or MRSA.
Active surveillance is key to the prevention of infectious disease, whether it is COVID-19, CRE or MRSA. Active surveillance and other preventative protocols are costly and staff intense. With lean pre-pandemic staffing, our private healthcare system did not have the infrastructure to withstand the onslaught of COVID-19 cases. Bacterial infection rates rose.
COVID-19 is not going away. We may well be entering a status quo or an endemic phase which requires providing services to a consistently high number of patients. With new variants constantly emerging and a significant segment of the United States population recalcitrant to public health advisements and vaccines, the United States Healthcare System will be under continued stress.
Risk adjustment should only be applied when effective strategies do not exist to prevent the occurrence of adverse outcomes. The question remains: Are we going to meet the challenge, build the needed infrastructure and strengthen our healthcare system to adapt to the new normal, or are we going to normalize deviance with continued lean staffing and just-in-time supply chains? I would choose the former and use financial incentives to drive the change.
[ad_2]
Source link